In the realm of dermatology, where skin conditions often present themselves as very complex puzzles, two distinct entities stand out: Erythema Multiforme and Erythema Migrans. While they share a similar abbreviation, these two conditions couldn’t be more different in terms of their underlying causes, pathophysiology, clinical presentations, and implications for patient care.
As we dive into this educational journey, allow me, a seasoned medical professional, to walk you through the key points that differentiate these two skin conditions. Beyond their mere names lies a tremendous wealth of knowledge that holds significance for healthcare professionals and individuals seeking a deeper understanding of these skin manifestations.
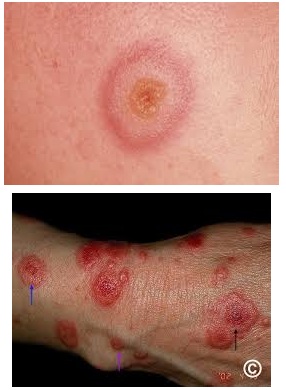
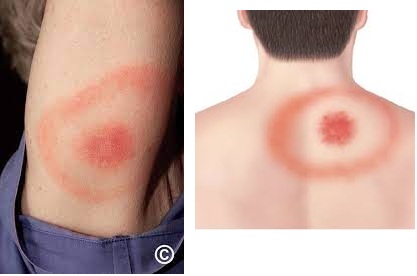
Erythema Multiforme, characterized by its enigmatic “target lesions”, often leaves patients and clinicians alike intrigued by its diverse triggers and potential complications if not treated soon. On the other hand, Erythema Migrans, synonymous with Lyme disease, is a dermatological sentinel, presents with a “bull’s-eye” appearing rash — a warning sign of a much larger systemic concern.
In this comprehensive blog post, we will dissect the clinical features, etiology, diagnostic approaches, treatment strategies, and potential complications associated with both Erythema Multiforme and Erythema Migrans. We hope that you find this blog post useful! 🙂
Erythema Multiforme vs Erythema Migrans
Below are the important differences between erythema multiforme and erythema migrans. All these points are high-yield for medical students and doctors. 🙂
| Characteristics | Erythema Multiforme | Erythema Migrans |
|---|---|---|
| Slide |
“A maculopapular rash appearing usually on palms and feet, often pruritic and blanches away slowly” |
“Bull’s-eye” appearance; central erythema and necrosis; expands rather than migrating. |
| Definition | Erythema Multiforme is an acute, immune-mediated skin disorder characterized by target-like lesions. It can be triggered by infections, drugs, or other factors (important causes have been discussed below). | Erythema Migrans is the characteristic skin rash associated with Lyme disease, caused by the spirochete bacterium Borrelia burgdorferi. It’s a red rash with a central clearing that looks like a “bull’s eye.” |
| Cause |
|
Bacterial Infection:
|
| Lesion Appearance | Target-like or iris lesions, with concentric rings of various colors (red, pale, and normal skin tone). | Circular or oval-shaped rash with central clearing, resembling a bull’s-eye. |
| Distribution of lesion | Can affect any part of the body, mainly the extremities, face, trunk, palms, and soles. | Typically occurs at the site of the tick bite and expands gradually over the period of time. |
| Systemic Symptoms | Can be associated with mild constitutional symptoms or mucous membrane involvement. | May be accompanied by flu-like symptoms such as fever, lethargy, fatigue, headache, and muscle aches. |
| Duration | Acute and self-limiting, with lesions resolving within weeks. | The rash can last for several weeks if left untreated. |
| Treatment | Depends on the underlying cause. Supportive care for mild cases; discontinuation of triggering medications. | Treatment usually involves antibiotics like Doxycycline or Amoxicillin for Lyme disease. |
| Complications | Can recur or progress to a more severe form called Stevens-Johnson syndrome or toxic epidermal necrolysis (TEN). | If left untreated, Lyme disease can lead to more serious systemic complications affecting the joints, heart, and nervous system. |
| Geographic Occurrence | Worldwide distribution. | Common in areas with high tick populations, particularly in warm regions of North America, Europe, and Asia. |
| Prevention | Avoidance of triggers (like certain infections or medications). | Prevent tick bites by wearing protective clothing, using insect repellents, and checking for ticks on clothing and body after outdoor activities. |
| Diagnostic Markers | Diagnosis is primarily clinical based on lesion appearance and patient history. |
Diagnosis is based on clinical signs, symptoms, and history of potential exposure to ticks in an endemic area. Laboratory tests like serology can confirm Lyme disease. |
Happy learning, everyone! 🙂

![Erythema Multiforme vs Erythema Migrans [High-yield Notes] Erythema Multiforme vs Erythema Migrans](https://www.medicosrepublic.com/wp-content/uploads/2023/08/Erythema-Multiforme-vs-Erythema-Migrans-High-yield-Notes-696x583.jpg)
![AIDS Defining Conditions Mnemonic with their CD4 Count [High-Yield] AIDS Defining Conditions Mnemonic](https://www.medicosrepublic.com/wp-content/uploads/2023/08/AIDS-Defining-Conditions-Mnemonic-with-CD4-Count-218x150.jpg)





![Gerstmann Syndrome Features Mnemonic [Easy-to-remember] Gerstmann Syndrome Features Mnemonic](https://www.medicosrepublic.com/wp-content/uploads/2025/06/Gerstmann-Syndrome-Features-Mnemonic-150x150.jpg)
![Cerebellar Signs Mnemonic [Easy to remember] Cerebellar Signs Mnemonic](https://www.medicosrepublic.com/wp-content/uploads/2025/06/Cerebellar-Signs-Mnemonic-150x150.jpg)
![Seizure Features Mnemonic [Easy-to-remember] Seizure Features Mnemonic](https://www.medicosrepublic.com/wp-content/uploads/2025/06/Seizure-Features-Mnemonic-1-150x150.jpg)

![Recognizing end-of-life Mnemonic [Easy to remember]](https://www.medicosrepublic.com/wp-content/uploads/2025/06/Recognizing-end-of-life-Mnemonic-150x150.jpg)
![Multi-System Atrophy Mnemonic [Easy-to-remember] Multi-System Atrophy Mnemonic](https://www.medicosrepublic.com/wp-content/uploads/2025/06/Multi-System-Atrophy-Mnemonic-150x150.jpg)
![How to Remember Southern, Northern, and Western Blot Tests [Mnemonic] How to Remember Southern, Northern, and Western Blot Tests](https://www.medicosrepublic.com/wp-content/uploads/2025/06/How-to-Remember-Southern-Northern-and-Western-Blot-Tests-150x150.jpg)